To prepare for 2021 open enrollment, group health plan sponsors should be aware of the legal changes affecting the design and administration of their plans for plan years beginning on or after Jan. 1, 2021. Employers should review their plan documents to confirm that they include these required changes.
In addition, any changes to a health plan’s benefits for the 2021 plan year should be communicated to plan participants through an updated summary plan description (SPD) or a summary of material modifications (SMM).
Health plan sponsors should also confirm that their open enrollment materials contain certain required participant notices, when applicable—for example, the summary of benefits and coverage (SBC). There are also some participant notices that must be provided annually or upon initial enrollment. To minimize costs and streamline administration, employers should consider including these resources in their open enrollment materials.
Plan Changes
ACA Affordability Standard
Under the ACA’s employer shared responsibility rules, applicable large employers (ALEs) are required to offer affordable, minimum value health coverage to their full-time employees (and dependent children) or risk paying a penalty. These employer shared responsibility requirements are also known as the “employer mandate” or “pay or play” rules.
Under the ACA, an ALE’s health coverage is considered affordable if the employee’s required contribution to the plan does not exceed 9.5% of the employee’s household income for the taxable year (as adjusted each year). The adjusted percentage is 9.78% for 2020.
For plan years that begin on or after Jan. 1, 2021, the affordability percentage is 9.83%. This means that employer sponsored coverage for the 2021 plan year will be considered affordable under the employer shared responsibility rules if the employee’s required contribution for self-only coverage does not exceed 9.83% of the employee’s household income for the tax year.
🗹 If you are an ALE, confirm that at least one of the health plans offered to full-time employees (and their dependent children) satisfies the ACA’s affordability standard (9.83% for 2021 plan years). Because the affordability percentage increased from 2020 when it was 9.78%, employers may have additional flexibility in setting their employee contributions for 2021 to avoid a penalty under the pay or play rules.
Out-of-Pocket Maximum
Non-grandfathered health plans are subject to limits on cost sharing for essential health benefits (EHB). The annual limit on total enrollee cost sharing for EHB for plan years beginning on or after Jan. 1, 2021, is $8,550 for self-only coverage and $17,100 for family coverage.
🗹 Review your plan’s out-of-pocket maximum to make sure it complies with the ACA’s limits for the 2021 plan year ($8,550 for self-only coverage and $17,100 for family coverage).
🗹 If you have a high deductible health plan (HDHP) that is compatible with a health savings account (HSA), keep in mind that your plan’s out-of-pocket maximum must be lower than the ACA’s limit. For 2021 plan years, the out-of pocket maximum limit for HDHPs is $7,000 for self-only coverage and $14,000 for family coverage.
🗹 If your plan uses multiple service providers to administer benefits, confirm that the plan coordinates all claims for EHB across the plan’s service providers or divides the out-of-pocket maximum across the categories of benefits, with a combined limit that does not exceed the maximum for 2021.
Preventive Care Benefits
The ACA requires non-grandfathered health plans to cover certain preventive health services without imposing cost sharing requirements (that is, deductibles, copayments or coinsurance) for the services. Health plans are required to adjust their first-dollar coverage of preventive care services based on the latest preventive care recommendations. If you have a non-grandfathered plan, you should confirm that your plan covers the latest recommended preventive care services without imposing any cost sharing.
More information on the recommended preventive care services is available through the U.S. Preventive Services Task Force and www.HealthCare.gov.
Health FSA Contributions
The ACA imposes a dollar limit on employees’ salary reduction contributions to a health flexible spending account (FSA) offered under a cafeteria plan. An employer may impose its own dollar limit on employees’ salary reduction contributions to a health FSA, as long as the employer’s limit does not exceed the ACA’s maximum limit in effect for the plan year.
The ACA set the health FSA contribution limit at $2,500. For years after 2013, the dollar limit is indexed for cost-of-living adjustments. For 2020 plan years, the health FSA limit is $2,750. The IRS has not yet announced the health FSA limit for 2021 plan years.
🗹 Watch for IRS guidance on the health FSA limit for 2021 plan years.
🗹 Once the 2021 health FSA limit is announced, confirm that your health FSA will not allow employees to make pre tax contributions in excess of that limit.
🗹 Communicate the health FSA limit to employees as part of the open enrollment process.
HDHP and HSA Limits for 2021
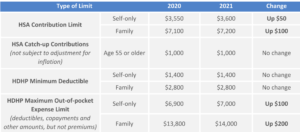
If you offer an HDHP to your employees that is compatible with an HSA, you should confirm that the HDHP’s minimum deductible and out-of-pocket maximum comply with the 2021 limits. The IRS limits for HSA contributions and HDHP maximum out-of-pocket limit increase for 2021. The HSA contribution limits will increase effective Jan. 1, 2021, while the HDHP out-of-pocket limit will increase effective for plan years beginning on or after Jan. 1, 2021.
🗹 Check whether your HDHP’s cost-sharing limits need to be adjusted for the 2021 limits.
🗹 If you communicate the HSA contribution limits to employees as part of the enrollment process, these enrollment materials should be updated to reflect the increased limits that apply for
2021.
The following table contains the HDHP and HSA limits for 2021 as compared to 2020. It also includes the catch-up contribution limit that applies to HSA-eligible individuals who are age 55 or older, which is not adjusted for inflation and stays the same from year to year.
Additional HRA Design Options
Employers have two additional health reimbursement arrangement (HRA) design options for plan years that begin on or after Jan. 1, 2020—an individual coverage HRA (ICHRA) and an excepted benefit HRA (EBHRA).
ICHRA
An ICHRA may be used to reimburse the cost of individual insurance premiums (and Medicare premiums) on a tax-preferred basis as an alternative to traditional group health plan coverage, subject to the following conditions:
- The ICHRA must require that the employee and any dependents are enrolled in individual health insurance (or Medicare) coverage for each month that the individual(s) are covered by the ICHRA;
- An employer that offers an ICHRA to any class of employees may not also offer a traditional group health plan to the same class of employees;
- If a plan sponsor offers an ICHRA to any class of employees, it must generally be offered on the same terms to all participants within the class;
- Participants must be allowed to opt out of and waive future reimbursements from the ICHRA once per plan year;
- The ICHRA must provide the written notice to each participant at least 90 days before the beginning of each plan year. A model notice is available for employers to use.
EBRHA
Employers offering traditional group health plan coverage may offer an EBHRA of up to $1,800 per year (indexed annually for inflation) to reimburse eligible employees for certain qualified medical expenses. An EBHRA must be offered in conjunction with a traditional group health plan, although employees are not required to enroll in the traditional plan to use the EBHRA. An EBHRA cannot reimburse premiums for individual health coverage, coverage under a group health plan (other than COBRA or other group continuation coverage), or Medicare Parts B or D.
🗹 Review the additional HRA design options and decide whether to adopt either of these options for your employees (or a group of your employees).
🗹 If you adopt an ICHRA for 2021, provide the required employee notice at least 90 days before the beginning of the plan year.
Wellness Plan Design—ADA Compliance
The Americans with Disabilities Act (ADA) applies to employer-sponsored wellness plans that ask for health information or include medical exams (for example, biometric testing). In May 2016, the Equal Employment Opportunity Commission (EEOC) issued final rules addressing the ADA’s requirements for employer-sponsored wellness programs. The final rules included a 30% limit for wellness incentives. A federal court vacated this incentive limit, effective Jan. 1, 2019. Consistent with this court ruling, the EEOC removed the incentive limit from its final wellness rules.
Due to the lack of guidance from the EEOC, it is currently unclear what level of incentive, if any, is permissible under the ADA for employer-sponsored wellness plans that ask for health information or include medical exams.
🗹 If you sponsor a wellness program that asks for health information or includes medical exams, you should carefully review any incentive associated with the program (due to the lack of guidance from the EEOC).
🗹 Watch for any developments related to the EEOC’s wellness rules.
🗹 If the EEOC issues proposed wellness rules before the start of the 2021 plan year, review your wellness incentives and consider whether to make any adjustments.
ACA Disclosure Requirements
Summary of Benefits and Coverage
The ACA requires health plans and health insurance issuers to provide an SBC to applicants and enrollees to help them understand their coverage and make coverage decisions. Plans and issuers must provide the SBC to participants and beneficiaries who enroll or re-enroll during an open enrollment period. The SBC also must be provided to participants and beneficiaries who enroll other than through an open enrollment period (including those who are newly eligible for coverage and special enrollees).
On Nov. 8, 2019, the Departments of Labor (DOL) and Health and Human Services (HHS) issued an updated template and related materials for the SBC. These materials are required to be used for plan years beginning on or after Jan. 1, 2021. This means that the updated template must be used for the 2021 plan year’s open enrollment period.
🗹 In connection with a plan’s 2021 open enrollment period, prepare to use the new SBC template and related materials. The SBC should be included with the plan’s application materials. If coverage automatically renews for current participants, the SBC must generally be provided no later than 30 days before the beginning of the new plan year.
🗹 For self-funded plans, the plan administrator is responsible for providing the SBC. For insured plans, both the plan and the issuer are obligated to provide the SBC, although this obligation is satisfied for both parties if either one provides the SBC. Thus, if you have an insured plan, you should confirm that your health insurance issuer will assume responsibility for providing the SBCs.
Grandfathered Plan Notice
If you have a grandfathered plan, make sure to include information about the plan’s grandfathered status in plan materials describing the coverage under the plan, such as SPDs and open enrollment materials. Model language is available from the DOL.
Notice of Patient Protections
Under the ACA, non-grandfathered group health plans and issuers that require designation of a participating primary care provider must permit each participant, beneficiary and enrollee to designate any available participating primary care provider (including a pediatrician for children). Also, plans and issuers that provide obstetrical/gynecological care and require a designation of a participating primary care provider may not require preauthorization or referral for obstetrical/gynecological care.
If a non-grandfathered plan requires participants to designate a participating primary care provider, the plan or issuer must provide a notice of these patient protections whenever the SPD or similar description of benefits is provided to a participant. If your plan is subject to this notice requirement, you should confirm that it is included in the plan’s open enrollment materials. Model language is available from the DOL.
Other Notices
Group health plan sponsors should consider including the following enrollment and annual notices with the plan’s open enrollment materials.
Initial COBRA Notice
The Consolidated Omnibus Budget Reconciliation Act (COBRA) applies to employers with 20 or more employees that sponsor group health plans. Group health plan administrators must provide an initial COBRA notice to new participants and certain dependents within 90 days after plan coverage begins. The initial COBRA notice may be incorporated into the plan’s SPD. A model initial COBRA notice is available from the DOL.
Notice of HIPAA Special Enrollment Rights
At or prior to the time of enrollment, a group health plan must provide each eligible employee with a notice of his or her special enrollment rights under the Health Insurance Portability and Accountability Act (HIPAA). This notice may be included in the plan’s SPD.
Summary Plan Description
Plan administrators must provide an SPD to new participants within 90 days after plan coverage begins. Any changes that are made to the plan should be reflected in an updated SPD booklet or described to participants through an SMM. Also, an updated SPD must be furnished every five years if changes are made to SPD information or if the plan is amended. Otherwise, a new SPD must be provided every 10 years.
HIPAA Privacy Notice
The HIPAA Privacy Rule requires covered entities (including group health plans and issuers) to provide a Notice of Privacy Practices (or Privacy Notice) to each individual who is the subject of protected health information (PHI). Health plans are required to send the Privacy Notice at certain times, including to new enrollees at the time of enrollment. Also, at least once every three years, health plans must either redistribute the Privacy Notice or notify participants that the Privacy Notice is available and explain how to obtain a copy.
Self-insured health plans are required to maintain and provide their own Privacy Notices. Special rules, however, apply for fully insured plans. Under these rules, the health insurance issuer, and not the health plan itself, is primarily responsible for the Privacy Notice.
Special Rules for Fully Insured Plans: The plan sponsor of a fully insured health plan has limited responsibilities with respect to the Privacy Notice.
∙ If the sponsor of a fully insured plan has access to PHI for plan administrative functions, it is required to maintain a Privacy Notice and to provide the notice upon request.
∙ If the sponsor of a fully insured plan does not have access to PHI for plan administrative functions, it is not required to maintain or provide a Privacy Notice.
A plan sponsor’s access to enrollment information, summary health information and PHI that is released pursuant to a HIPAA authorization does not qualify as having access to PHI for plan administration purposes.
Model Privacy Notices are available through HHS.
Annual CHIPRA Notice
Group health plans covering residents in a state that provides a premium subsidy to low-income children and their families to help pay for employer-sponsored coverage must send an annual notice about the available assistance to all employees residing in that state. The DOL has provided a model notice.
WHCRA Notice
Plans and issuers must provide notice of participants’ rights to mastectomy-related benefits under the Women’s Health and Cancer Rights Act (WHCRA) at the time of enrollment and on an annual basis. Model language for this disclosure is available on the DOL’s website.
Medicare Part D Notices
Group health plan sponsors must provide a notice of creditable or non-creditable prescription drug coverage to Medicare Part D-eligible individuals who are covered by, or who apply for, prescription drug coverage under the health plan. This creditable coverage notice alerts the individuals as to whether or not their prescription drug coverage is at least as good as the Medicare Part D coverage. The notice generally must be provided at various times, including when an individual enrolls in the plan and each year before Oct. 15 (when the Medicare annual open enrollment period begins). Model notices are available on the Centers for Medicare and Medicaid Services’ website.
Summary Annual Report
Plan administrators who are required to file a Form 5500 must provide participants with a narrative summary of the information in the Form 5500, called a summary annual report (SAR). A model notice is available from the DOL.
Group health plans that are unfunded (that is, benefits are payable from the employer’s general assets and not through an insurance policy or trust) are not subject to the SAR requirement. The plan administrator generally must provide the SAR within nine months of the close of the plan year. If an extension of time to file the Form 5500 is obtained, the plan administrator must furnish the SAR within two months after the close of the extension period.
Michelle’s Law Notice
Group health plans that condition dependent eligibility on a child’s full-time student status must provide a notice of the requirements of Michelle’s Law in any materials describing a requirement for certifying student status for plan coverage. Under Michelle’s Law, a plan cannot terminate a child’s coverage for loss of full-time student status if the change in status
is due to a medically necessary leave of absence. Due to the ACA’s age 26 mandate for dependent coverage, most health plans no longer condition dependent eligibility on full-time student status and, thus, are not subject to Michelle’s Law.
HIPAA Opt-out for Self-funded, Nonfederal Governmental Plans
Sponsors of self-funded, nonfederal governmental plans may opt out of certain federal mandates, such as the mental health parity requirements and the WHCRA coverage requirements. Under an opt-out election, the plan must provide a notice to enrollees regarding the election. The notice must be provided annually and at the time of enrollment. Model language for this notice is available for sponsors to use.
Wellness Program Notices
Group health plans that include wellness programs may be required to provide certain notices regarding the program’s design. As a general rule, these notices should be provided when the wellness program is communicated to employees and before employees provide any health-related information or undergo medical examinations.
🗹 HIPAA Wellness Program Notice—HIPAA imposes a notice requirement on health-contingent wellness programs that are offered under group health plans. Health-contingent wellness plans require individuals to satisfy standards related to health factors (for example, not smoking) in order to obtain rewards. The notice must disclose the availability of a reasonable alternative standard to qualify for the reward (and, if applicable, the possibility of waiver of the otherwise applicable standard) in all plan materials describing the terms of a health-contingent wellness program. The DOL’s compliance assistance guide includes a model notice that can be used to satisfy this requirement.
🗹 ADA Wellness Program Notice—Employers with 15 or more employees are subject to the ADA. Wellness programs that include health-related questions or medical exams must comply with the ADA’s requirements, including an employee notice requirement. Employers must give participating employees a notice that tells them what information will be collected as part of the wellness program, with whom it will be shared and for what purpose, the limits on disclosure and the way information will be kept confidential. The EEOC has provided a sample notice to help employers comply with this ADA requirement.
LINKS AND RESOURCES
∙ Revenue Procedure 2020-32, which includes the inflation adjusted limits for HSAs and HDHPs for 2021
∙ Model notices for group health plans, including the Women’s Health and Cancer Rights Act (WHCRA) Notice
∙ Model COBRA notices for group health plans
For any questions regarding the article or 2021 Open Enrollment, please email info@benefitsqb.com or schedule a call with us today!
This Compliance Overview is not intended to be exhaustive nor should any discussion or opinions be construed as legal advice. Readers should contact legal counsel for legal advice. ©2020 Zywave, Inc. All rights reserved.